Pregnancy and Birth - Real-life applications
Changing Views on Childbirth
Before modern times, the realm of childbirth was a world exclusive to women, and few men ever entered the birth chamber. It was a place of excruciating pain and serious danger to the mother giving birth, so filled with blood and screaming that few men would have dared enter even if they had wanted to do so. Women had to give birth without anesthesia and any number of other amenities of modern medical care, including sophisticated diagnostic techniques and equipment, such as ultrasound, as well as antiseptic environments and surgical techniques, such as cesarean section.
In those days, birthing assistance was the work of midwives, women who lacked formal schooling in medicine (which was unavailable to most women in any case) but made up in experience for what they lacked in education. By about 1500, however, as medicine began to progress after many centuries of stagnation, male doctors increasingly forced midwives out of a job. In 1540 the European Guild of Surgeons declared that "no carpenter, smith, weaver, or woman shall practice surgery." A major turning point in the male takeover of birthing assistance duties came with the invention of the forceps, tong-like instruments that could be used for extracting a baby during difficult births. The inventor was the English obstetrician (a physician concerned with childbirth) Peter Chamberlen the Elder (1560-1631), and he and his descendants for a century closely guarded the design of the brilliant invention. Even the mothers on whom it was used never saw the instrument, and midwives were prohibited from using forceps to assist during childbirth.
OBSTETRICIANS TAKE OVER.
By the eighteenth century, however, Chamberlen's descendants had released their exclusive claim over the forceps, and use of the instrument spread to other medical professionals. This gave male obstetricians a great technological advantage over female midwives and further ensured the separation of the midwives from the medical profession. By 1750 numerous physicians and surgeons had gained the status of "man-mid-wives," and the growth of university courses on obstetrics established it as a distinct medical specialty. By the latter part of the 1700s, most women of the upper classes had come to rely on professionally trained doctors rather than midwives, yet in America, where doctors were scarcer than in Europe, the profession of midwife continued to flourish into the 1800s. Still, by the early twentieth century, childbirth had moved out of the home and into the hospital, and at mid-century it had become a completely medical process, attended by physicians and managed with medical equipment and procedures, such as fetal monitors, anesthesia, and surgical interventions.
THE REACTION IN THE LATE TWENTIETH CENTURY.
Many women of the late twentieth century found themselves dissatisfied with this clinical approach to childbirth. Some believed that the medical establishment had taken control of a natural biological process, and women who wanted more command over labor and delivery helped popularize new ideas on childbirth that sought to reduce or eliminate medical interventions. Today, some women choose to deliver with the help of a nurse-midwife, who, like her premodern counterparts, is trained to deliver babies but is not a doctor. There are women who even choose home birth, attended by a doctor or midwife or sometimes both. There are even brave souls who, in the face of increasing concern about the effect of anesthesia on the fetus, refuse artificial means of controlling pain and instead rely on breathing and relaxation techniques. For the first time in many years, the screams of women giving birth "naturally" once again filled the halls of hospital maternity wards and home birthing rooms.
Modern Childbirth
The last few paragraphs represent an extreme reaction—a view not shared by many women, who have been more than happy to avail themselves of the benefits of childbirth in the modern world. Such benefits include an epidural, a type of anesthetic procedure that serves to alleviate the pain of parturition, or childbirth, while making it possible for the mother to remain conscious. Still, even for women who have no interest in giving birth at home or without the aid of drugs, much has changed in the world of childbirth. Women may choose a happy medium between the medical establishment and more traditional methods, for instance, by opting to consult with an obstetrician and a midwife.
Today, many obstetricians are women. This has had an incalculable effect on making childbirth psychologically easier for many women: though some are happy to retain a male obstetrician, many others find themselves much more comfortable being cared for by a physician who, in all likelihood, has given birth herself. The increasingly important role of the female obstetrician, along with other factors, serves to symbolize the fact that the world has progressed beyond the old false dilemma between medical care from a male or a female, between medicine and nature, between hospital and home.
A HOSPITAL AS HOME.
Hospital rooms, in fact, are starting to resemble rooms at home. Everywhere one looks in the modern maternity environment, there is evidence that much has changed, not only from the very old days, when male doctors were not involved in childbirth at all, but also from the more recent past, when males took over the process entirely. In a brilliant innovation, many hospitals have created a situation in which the woman gives birth in her own hospital room, which is outfitted with couches, cabinets, curtains, and rocking chairs to make it look like a home rather than a hospital. To emphasize the smooth transition between home life and the delivery room, fathers, once banished from the labor and delivery chambers, now are welcomed as partners in the birth process.
A father may even cut the umbilical cord, and he is certainly likely to be in the delivery room with a video camera, recording the event for posterity—yet another change from the past. Fathers are not the only ones filming in the delivery room. Today, cable television networks, such as the Learning Channel, provide programming that offers a frank view of the delivery process, complete with candid footage that sometimes can be as dramatic as it is revealing. The maternity ward, once a closed place, has increasingly become an open book.
Saving and Improving Lives
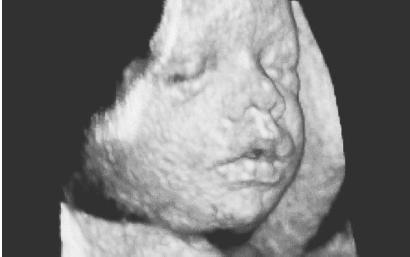
Many a mother and father alike can breathe a prayer (or at least a sigh) of thanks for all the innovations that today make birth much safer than it once was. Among them are a variety of techniques for embryo and fetal diagnosis, which help make parents aware of possible problems in the growing embryo. Ultrasound diagnosis, a technique similar to that applied on submarines for locating underwater structures, uses high-pitched sounds that cannot be heard by the human ear. These sounds are bounced off the embryo, and the echoes received are used to identify embryonic size.
By the eighteenth week of pregnancy, ultrasound technology can detect many structural abnormalities, such as spina bifida (various defects of the spine), hydrocephaly (water on the brain), anencephaly (no brain), heart and kidney defects, and harelip (in which the upper lip is divided into two or more parts). On a less dire and much more pleasant note, it can also give future parents an opportunity to gain their first glimpse of their child, and an experienced ultra-sound technician usually can tell them the baby's sex if they choose to learn it before the birth.
PRENATAL TESTING.
Chorionic villi sampling is the most sophisticated modern technique used to assess possible inherited genetic defects. This test typically is performed between the sixth and eighth week of embryonic development. During the test, a narrow tube is passed through the vagina or the abdomen, and a sample of the chorionic villi (small hairlike projections on the covering of the embryonic sac) is removed while the physician views the baby via ultrasound.
Chorionic villi are rich in both embryonic and maternal blood cells. By studying them, genetic counselors can determine whether the baby will have any of several defects, including Down syndrome (characterized by mental retardation, short stature, and a broadened face), cystic fibrosis (which affects the digestive and respiratory systems), and the blood diseases hemophilia, sickle cell anemia, and thalassemia. (Several of these disorders are discussed in different essays throughout this book; for instance, Down syndrome is examined in Mutation.) As with ultrasound, it also can show the baby's gender.
Another important form of prenatal (before the birth of the child) testing is amniocentesis, performed around week 16, in which amniotic fluid is drawn from the uterus by means of a needle inserted through the abdomen. Amniocentesis, too, can reveal the sex of the child, as well as a host of genetic disorders such as Tay-Sachs disease, cystic fibrosis, and Down syndrome. However, amniocentesis involves the risk of fetal loss as a result of disruption of the placenta. Chorionic villi sampling is even more risky, with an even higher possibility of fetal loss than amniocentesis, probably because it is conducted at an earlier stage.
In alpha-fetoprotein screening, which takes place somewhere between the 16th and 18th weeks, proteins from the amniotic sac and the fetal liver are taken as a means of screening for specific defects. Because of uncertainties involved in interpretation of the results, alpha-fetoprotein screening is not a common procedure.
CESAREAN SECTION.
Another extremely important technique that has saved the life of many babies and mothers is cesarean section. The normal position for a baby in delivery is head first; when a baby is in the breech position, with its bottom first, it poses grave dangers to both the mother and the child. Not only could the baby fail to emerge in time to begin breathing normally, thus running the risk of brain damage, but it also can become stuck, endangering the life of the mother. Today these dangers are overcome by such techniques as turning the baby and by cesarean section, an operation in which the baby is removed via surgery from the mother's abdomen. Cesarean sections may also be performed due to other complications, including fetal and/or maternal distress.
The term cesarean refers to the Roman emperor Julius Caesar (102-44 B.C. ), who supposedly was delivered in this fashion. But the story of Caesar's birth is undoubtedly a legend: until the early modern era, cesarean sections were performed only to save a living baby after the mother had died in childbirth. The reason is that cesareans were likely to be fatal to the mother. Only in the late nineteenth century, by which time doctors had come to understand the importance of providing an antiseptic or germ-free environment, did cesarean sections become practical. Today the C-section, as it is called, has become a routine procedure—one that has saved literally hundreds of thousands, perhaps millions, of lives.
WHERE TO LEARN MORE
Assisted Reproduction Foundation (Web site). <http://www.reproduction.org/> .
Bainbridge, David. Making Babies: The Science of Pregnancy. Cambridge, MA: Harvard University Press, 2001.
Facts About Multiples (Web site). <http://mypage.direct.ca/c/csamson/multiples.html> .
Midwifery, Pregnancy, Birth and Breastfeeding (Web site). <http://www.moonlily.com/obc/> .
Pence, Gregory E. Who's Afraid of Human Cloning? Lanham, MD: Rowman and Littlefield, 1998.
Pregnancy and Birth (Web site). <http://pregnancy.about.com/mbody.htm> .
Pregnancy and Reproduction Topics. Medline/National Library of Medicine, National Institutes of Health (Web site). <http://www.nlm.nih.gov/medlineplus/pregnancyandreproduction.html> .
Rudy, Kathy. Beyond Pro-Life and Pro-Choice: Moral Diversity in the Abortion Debate. Boston: Beacon Press, 1996.
Vaughan, Christopher C. How Life Begins: The Science of Life in the Womb. New York: Times Books, 1996.
Comment about this article, ask questions, or add new information about this topic: