Contraception
Contraception, also called birth control, is the deliberate effort to halt conception a child (to keep a woman from becoming pregnant). Attempts to prevent pregnancy date back to ancient times and cultures. Some form of contraception is used by more than half the women in the United States. Although widespread, contraception remains controversial, with some religious and political groups opposed to distribution of contraceptives.
Ancient methods in use today
Some early methods of contraception involved techniques still used today. Gum arabic—a substance with which Egyptians coated tampons to kill sperm—is used to make spermicides contained in modern contraceptive jellies and foams. The ancient practice of prolonged nursing of infants to prevent conception of future children remains in current use, although it is by no means 100 percent effective. The modern diaphragm has its origin in a device made from bamboo that Asian women used as a barrier to the cervix (the opening to the uterus, or womb). The Chinese promoted "coitus interruptus," the withdrawal of the man's penis from the woman's vagina before ejaculation. Probably the most common contraceptive method in the world, this practice has resulted in numerous accidental pregnancies. The rhythm method (in which intercourse is avoided on the days of the month when a woman is most likely to become pregnant) was and remains the only form of birth control approved by the Roman Catholic Church.
Words to Know
Fallopian tube: One of a pair of structures in the female reproductive system that carries eggs from the ovaries to the uterus.
Fertilization: The union of an egg and sperm to form a new individual.
Hormone: A chemical messenger or substance produced by the body that has an effect on organs in other parts of the body.
Ovary: One of a pair of female reproductive organs that produces eggs and female sex hormones.
Ovulation: The release of an egg, or ovum, from an ovary.
Ovum: A mature female sex cell produced in the ovaries.
Sperm: A mature male sex cell secreted in semen during male ejaculation.
Uterus: The female organ in which the fetus develops before birth.
Evolution of the condom
The practice of using condoms to prevent pregnancy and sexually transmitted diseases began in the sixteenth century, when cloth condoms were promoted to protect against syphilis. By the eighteenth century, condoms were made of animal membrane, making them waterproof and more effective as birth control devices. Latex (rubber) condoms were first produced during the Industrial Revolution (about 1750 to about 1850). The emergence of acquired immunodeficiency syndrome (AIDS) in the 1980s again resulted in the widespread promotion of condom use as an effective barrier to disease.
Modern methods of contraception
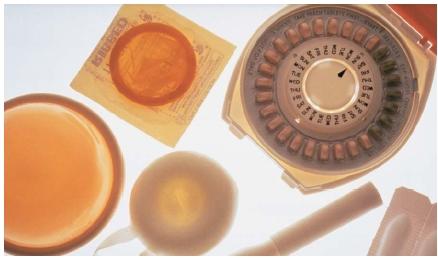
Contraceptive devices that were developed in the late nineteenth century and are still used today include the diaphragm, a rubber cap that fits over the cervix and prevents the passage of sperm into the uterus; the contraceptive sponge, also a device used to cover the cervix before sexual intercourse; and foams and jellies containing spermicides that are inserted into the vagina before intercourse.
Advances in medical knowledge led to the development in the 1960s of the IUD (or intrauterine device), which is placed in the uterus to prevent or interrupt the process of conception. Birth control pills, approved for use in 1960 and the most popular contraceptive in the United States, contain hormones that are released into a woman's system on a regular basis (some are taken 21 days per month, others are taken every day) to prevent pregnancy. Different pills act in different ways: some inhibit ovulation (the release of an egg from the ovary), some prevent implantation
of a fertilized egg (thereby denying cells the nourishment they need to develop into an embryo), and some thicken the secretions throughout the woman's reproductive system so that her partner's sperm has less of a chance to meet her egg.
Other recent developments include a matchsticklike device that is implanted under the skin of a woman's upper arm; it lasts about five years, releasing a contraceptive into the bloodstream that inhibits ovulation. An injectable form of contraceptive provides protection from pregnancy for three months at a time, but the most common reported side effects—including significant weight gain and mood swings—make this an unattractive choice for many women. In addition, a condom that can be inserted into the vagina of females became available in the mid-1990s, but its effectiveness is still being debated.
In 2000, in a landmark decision that received both widespread praise and protest, the U.S. Food and Drug Administration (FDA) approved the marketing of an abortion-inducing pill. This was the first alternative to surgical abortion approved in the United States. The prescription drug, called mifepristone or RU-486, was first developed in France in 1980. As of the end of 2000, 16 countries around the world had approved its use.
An abortion using mifepristone takes place in three steps. First, in a doctor's office, a woman is given a pregnancy test. If she is pregnant and it has been no longer than seven weeks since her last menstrual period, she is given three pills of mifepristone. The drug blocks the hormone progesterone, which is required to maintain a pregnancy. The woman then returns to the doctor's office within two days to take two tablets of a second drug, misoprostol. This second drug is a hormonelike substance that causes a woman's uterus to contract, expelling the fetal tissue, usually within six hours of taking the drug. Fourteen days later, she returns to her doctor's office and is checked to make sure she is no longer pregnant and no fetal tissue remains in her uterus. About 5 percent of the time, the abortion is incomplete and a woman will have to have a surgical abortion. Mifepristone fails completely in about 1 percent of the women who take it. The side effects of this abortion procedure are similar to a spontaneous miscarriage: uterine cramping, bleeding, nausea, and fatigue.
Sterilization
Sterilization, the surgical alteration of a male or female to prevent them from bearing children, is the most common form of birth control for women in the United States. In men, the operation is called a vasectomy. It is a simple out-patient procedure that involves snipping the vessel through which sperm passes so that semen—the off-white secretion ejected from the penis at the time of sexual climax—no longer contains sperm.
In women, sterilization involves a procedure called tubal ligation, in which the fallopian tubes that carry eggs from the ovaries to the uterus are tied or clipped. An egg that is released by an ovary during ovulation does not reach the uterus, thus preventing fertilization.
Challenges of contraception
Developing a foolproof method of birth control that has little or no side effects, is simple to use, and is agreeable to both men and women is a challenge. Sterilization is such a method, but only if the person undergoing the operation no longer wants to bear children.
Unwanted pregnancies can be measured by the rate of abortion (the ending of a pregnancy). Although many women who undergo abortions do not practice birth control, some pregnancies are the result of contraceptive failure. Abortion rates typically are highest in countries where contraceptives are not readily available. Some experts believe that easier access to contraceptive services would result in lower rates of accidental pregnancy and abortion.
[ See also Fertilization ; Reproduction ]
I work for a research organization that studies sexual and reproductive health. I'm interested in getting permission to use the photo of contraceptive methods that you used on your website under "Contraception."
Can you please send me the contact information of the photo owner?
Thanks,
Elizabeth