Schizophrenia

Schizophrenia (pronounced skiht-zo-FREH-nee-uh) is a severe mental condition that interferes with normal thought processes, causing delusions, hallucinations, and mental disorganization. As the most common of the extremely serious mental disorders known as psychosis (pronounced sy-KO-sis), it affects men and women equally, is found all over the world, and is usually a long-term illness with no definite cure.
Its victims
Schizophrenia is described by the National Institute of Mental Health (NIMH) as a "chronic, severe, and disabling brain disease." NIMH estimates that approximately 1 percent of the American population at some point suffers from schizophrenia, meaning that more than two million Americans are considered to be schizophrenic in any given year. Others estimate that as many as half the patients in U.S. mental hospitals are schizophrenics. Although it occurs in women as often as in men, it seems to appear earlier in men, usually in their late teens or early twenties. Very young people, however, can sometimes be affected.
To be schizophrenic is to suffer from a profound disruption of cognition, meaning that the schizophrenic individual has a major problem with knowing and thinking. Some describe this condition as a thought disorder, and once we understand the sometimes terrifying symptoms that schizophrenics experience in their minds, we can better see why their perception of reality is often a distorted one. The mental disturbances they experience also affect their emotions, their actions, and even their language. People with schizophrenia often do not see or experience things the way most people do, and their world is often one of delusions and hallucinations. It is not unusual for them to hear "voices" or see things that are not really there. A common delusion or false personal belief of schizophrenics is that someone or something is controlling their thoughts or plotting against them. Hallucinations are false sensory experiences; a person experiencing hallucinations thinks he or she is seeing, hearing, or even touching something that in reality is not there or does not exist.
Delusions and hallucinations
Once we understand what schizophrenics are experiencing mentally, we should not be surprised when their behavior becomes strange or even bizarre. Often they are fearful and withdrawn, but other times their actions and speech can be frightening or at least very confusing to others. Other recognizable symptoms of schizophrenia are socially inappropriate behavior, dulled emotional responses, isolation and withdrawal that suggest a loss of any social interests, an inability to concentrate or "think straight," and a loss of a sense of self as a unique and separate individual. Since schizophrenics experience hallucinations and delusions of all sorts, they are often very frightened, anxious, and confused people. At times they may act totally detached and remote, sitting rigid for hours. Other times they may be highly agitated, moving constantly. They are understandably difficult to be with and are just as difficult to treat.
Words to Know
Delusions: Incorrect beliefs about reality that are clearly false.
Hallucinations: Images, sounds, or odors that are seen, heard, or smelled by a person, but do not exist in reality.
Neurosis: Any emotional or mental disorder that affects only part of the personality, such as anxiety or mild depression, as a result of stress.
Neurotransmitter: A chemical that transmits electrical impulses (information) between nerve cells or nerve and muscle cells.
Psychosis: A major psychiatric disorder characterized by the inability to tell what is real from what is not real.
Historical evidence
Although some argue that schizophrenia is a modern disease, most agree that there is sufficient historical evidence to suggest that it is as old as humans. Stories of "mad" people whose behavior was beyond the limits or control of others and whose behavior was bizzare and unexplainable are found throughout the ancient history of all cultures. Ancient Babylonian documents are said to contain such evidence, and nearly 2,500 years ago, Greek historian Herodotus (480–425 B.C. ) described the mad king of Sparta. In the second century A.D. , Roman writer Celsus described three types of insanity, one of which sounds very much like schizophrenia. Many believe that schizophrenia was clearly described during the Middle Ages (period in European history from about A.D. 500 to 1500), and by the sixteenth century there are published accounts of clearly schizophrenic cases called "mania" or "melancolia." Some writers claim that the first printed description of schizophrenia was given by British physician Thomas Willis (1621–1675) when he described a certain type of "dementia."
Most agree, however, that the first modern description of symptoms now recognized as schizophrenia was given by German psychiatrist Emil Kraepelin (1856–1926) in 1896. Kraepelin's main contribution was his classification of mental illnesses, and it was Kraepelin who pointed out the difference between what is recognized today as manic-depressive psychosis and schizophrenia, which he called "dementia praecox" (pronounced deh-MEHN-shia PREE-cocks).
It was another German psychiatrist, however, who actually first suggested the term schizophrenia for the disease. In 1908, Eugen Bleuler (1857–1939) used the word schizophrenia in a paper he had written that was based on a study of 647 patients. Bleuler, who was a colleague of Austrian psychoanalyst Sigmund Freud (1856–1939), came up with the name to describe what he said was some sort of split in the proper functioning of the brain. He used the word split because he said that a schizophrenic's
ideas are often isolated or separate from his feelings. Bleuler's new name for this condition was therefore derived from the Greek words for "split" and "mind" and soon replaced the older term dementia praecox. It should be noted, however, that schizophrenia is neither a condition exhibiting a "split personality" nor one of "multiple personalities." Rather, these rare conditions are considered to be a type of neurosis (pronounced nur-OH-sis) that is a less severe emotional disorder.
Types of schizophrenia
The main difference between schizophrenia and any other type of neurosis is that a neurosis is an emotional disorder, whereas schizophrenia is considered a form of organic brain disease, meaning that there is a physical (and not an emotional) reason why something is wrong. Until recently, science could only describe or categorize the different types of schizophrenia, and the categories offered by Kraepelin are still used. Paranoid schizophrenics typically suffer from delusions of persecution; the hebephrenic (pronounced hee-beh-FREN-ik) type has very disorganized thinking, difficulty in communicating, and shows inappropriate emotional responses (like laughing at a funeral); the catatonic schizophrenic suffers from uncontrollable bodily movements. In reality, many schizophrenics often display symptoms from each type.
Causes
Although there are a number of competing theories as to the causes of schizophrenia, no one explanation has yet been proven. Unfortunately, this means that there is no known single cause of schizophrenia. That does not mean, however, that science is completely baffled and helpless in trying to understand this brain disease. Some of the early, more psychoanalytical explanations suggested that people who lacked affection during infancy and early childhood became schizophrenic, but these psychological theories could not be proven.
Science then naturally moved to seek more physical explanations, and with twenty-first century advances in biomedical research and advanced imaging technologies, most theories now have a basis in biology. That is, they seek to find the primary cause or causes of schizophrenia in the body itself, specifically in the brain. For example, it has long been known that schizophrenia runs in families, and that individuals with a close relative who suffered from the disease have a greater chance of developing it than people who have no relatives with the illness. This suggests that there are some genetic factors involved, and that perhaps a genetic predisposition (a tendency toward something) makes some more susceptible than others. In fact, research on the human genome, which is the complete collection of genes found in a single set of human chromosomes, suggests that the defect may be found somewhere on chromosomes 13 and 6, although this has not yet been proven conclusively.
Despite this possible genetic link, scientists know for many reasons that genes cannot be the sole cause of schizophrenia. A good proof of this is a set of identical twins, only one of whom suffers from schizophrenia. More likely, schizophrenia does not have a single cause, but instead is determined by a combination of biological factors. Another major avenue of investigation is in the chemistry of the brain. This new research focuses on the brain's neurotransmitters (pronounced ner-o-trans-MIH-terz), which are substances that allow the neurons or nerve cells to communicate with one another. Investigators are therefore concentrating on the neurotransmitters called dopamine (pronounced DOPE-uh-meen) and glutamate (pronounced GLUE-tuh-mait) to find if too much or too little is important to schizophrenia.
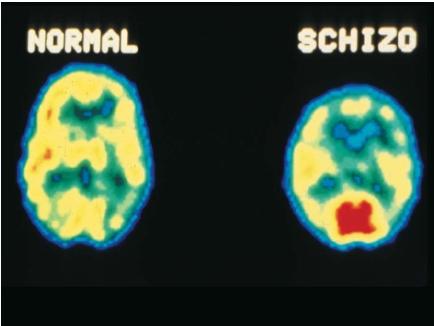
Other scientists are using new brain-imaging techniques to examine the brains of living schizophrenics to try to find abnormalities in structure or function. They now know, for example, that schizophrenics have enlarged ventricles, which are fluid-filled cavities inside the brain. Another brain-related theory is that schizophrenia is caused by some sort of developmental disorder that happened when the fetus was still growing inside the mother's womb. Some suggest that this damage may stay hidden or dormant until puberty, when the brain's normal changes somehow activate them. Finally, another theory is that the disease is caused by a slow-acting virus.
Treatment
Since schizophrenia has no one known cause, the best medicine can do is to treat the symptoms. Before the 1950s, electroconvulsive treatment or shock therapy was the only known method of treatment. Since that time, various drugs have been used to try to minimize the symptoms of schizophrenia. Reserpine was the first drug to work, and it was based on a plant used in folk medicine to treat insomnia and insanity. Later, the new drug named Thorazine was developed. Both it and Reserpine were found to work by blocking the neurotransmitter dopamine. In the 1990s, a new group of antipsychotic drugs were produced that were very effective in keeping delusions and hallucinations under control, but they also left their patients emotionally empty and even reduced their normal motivation.

Today, doctors are able to give new antipsychotic drugs in more calibrated or finely-tuned dosages so that they work to minimize the terrors, but do not put the person in a complete "emotional straitjacket." With their "demons" under better control, schizophrenics are able to deal with the everyday world in a more rational way. The key to every schizophrenic's health is to keep strictly to his or her treatment plan. However, although these new drugs are far better than the old ones, they still pose a long-term risk that the patient may develop serious side-effects involving the muscles.
Despite all the treatment, research, and gains in understanding, the fact remains that today's treatment for schizophrenia has limits. Very often, no matter how symptom-free the patient is, he or she may still have problems being "normal" in ways that matter—like caring for themselves, communicating with others, being motivated, and most important of all, establishing and keeping relationships with other people. It has been shown, however, that for patients whose symptoms are under control, the help and understanding they receive from their family, friends, and even self-help and support groups goes a long way toward making them better able to manage their condition. Continued understanding is needed as much as continued research.
[ See also Psychiatry ; Psychosis ; Tranquilizer ]
great source of information.
i know now everything there is to know about Schizophrenia.
ignore the comment above.
Stacy:)
thanks
David Lee
Student
Axia College
University of Phoenix